Psoriasis is a chronic inflammatory skin condition driven by immune system activity that affects how skin cells grow and shed. In people with psoriasis, skin cells are produced more rapidly than usual, leading to the build-up of thickened, inflamed patches on the skin.
Beyond visible skin changes, psoriasis can have a broader impact on daily life. Persistent itch, discomfort, and involvement of visible or sensitive areas may affect sleep, work, and social interactions. Many individuals experience periods of flare-ups that can last weeks or even months, followed by intervals of improvement. The unpredictable nature of these flares can be challenging to manage.
Understanding individual triggers plays an important role in managing psoriasis. Identifying factors such as stress, infections, medications, or skin injury may help reduce flare frequency and support better symptom control alongside medical treatment.
At Auria Dermatology Clinic, we assess and manage different forms of psoriasis. A structured dermatological evaluation helps determine the type of psoriasis involved and guides appropriate management.
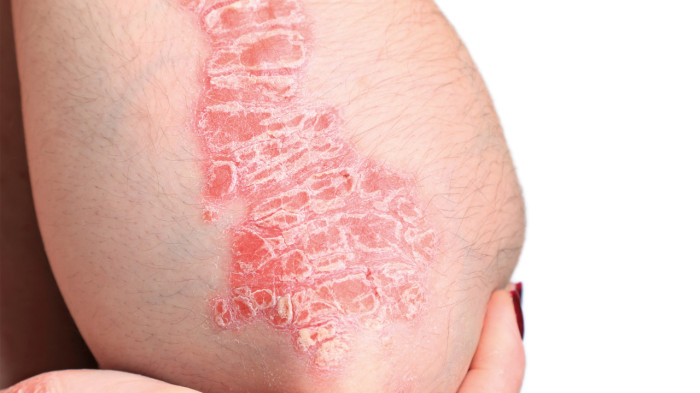
Plaque psoriasis is the most common form of psoriasis. It is characterised by well-defined areas of inflamed skin caused by increased skin cell turnover and immune system activity. The condition tends to follow a chronic relapsing course, with periods of improvement and flare-ups.
Affected skin typically appears as pink plaques covered with silvery or white scales. These patches are often found on the elbows, knees, scalp, lower back, and trunk. Some individuals experience itch, tightness, or cracking of the skin, particularly during flares.
Concerns are often related to visibility of lesions, discomfort, and unpredictability of flare-ups.
Psoriasis is associated with genetic predisposition and immune system dysregulation. Triggers that may worsen symptoms include infections, stress, skin injury, certain medications, and environmental factors.
Management is tailored to disease severity and affected areas and may include:
Systemic treatments, including oral or injectable immunomodulatory medications and biologics, for moderate to severe psoriasis
Inverse psoriasis affects skin folds, such as the armpits, groin, under the breasts, and around the genitals. Friction and moisture influence how the condition appears in these areas. Discomfort, soreness, or irritation may be delibitating, especially in warm or humid conditions and may be aggravated by sweating, friction, and secondary infections.
Psoriasis affecting the scalp may extend beyond the hairline and can be mistaken for dandruff. Treatment often involves medicated shampoos and topical scalp treatments.
Nail involvement may cause pitting, discolouration, thickening, or separation of the nail from the nail bed. Nail changes can occur with or without skin involvement.
This type affects the palms and soles, leading to thickened skin, scaling, and fissures that may interfere with daily activities.
Management for these forms is individualised and based on severity and functional impact.
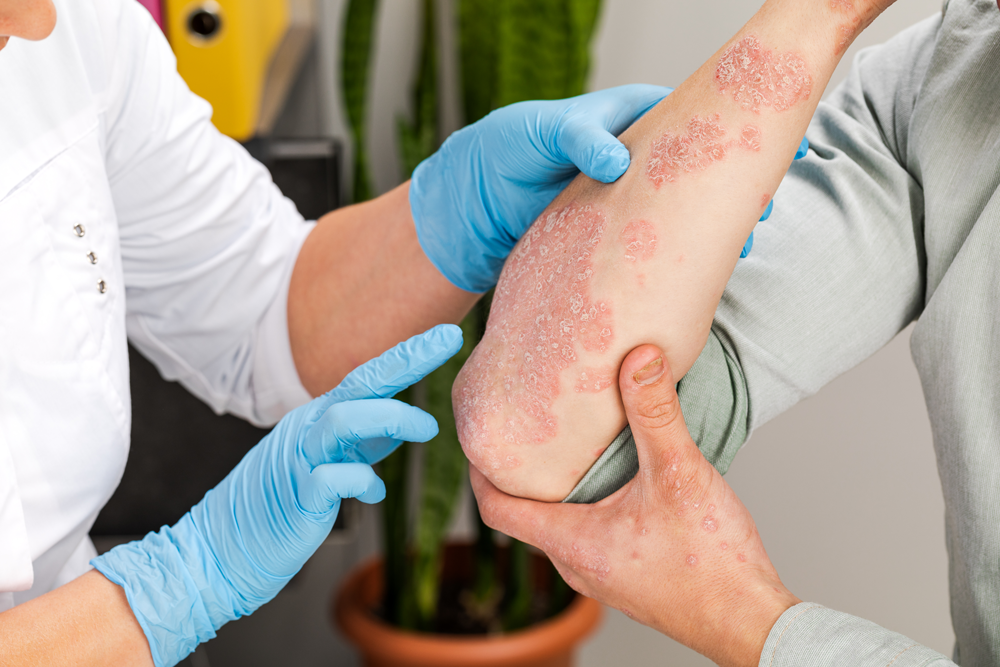
Psoriasis is usually diagnosed based on a combination of medical history and physical examination. A dermatologist will assess the appearance, distribution, and characteristics of the skin changes to help distinguish psoriasis from other inflammatory skin conditions.
In most cases, psoriasis can be diagnosed clinically. A skin biopsy may be recommended if the presentation is atypical or if there is uncertainty about the diagnosis. Blood tests are not routinely required but is useful to assess for metabolic disease in patients with chronic psoriasis.
An accurate diagnosis helps guide appropriate treatment and allows management to be tailored to the type and severity of psoriasis.

You may consider seeing a dermatologist if you experience:
A consultation with Dr Laura Hui allows for accurate diagnosis and discussion of suitable management approaches.
No. Psoriasis is not an infection and cannot be spread through contact.
Psoriasis is an immune-mediated condition in which the immune system plays a role in driving skin inflammation.
In some individuals, psoriasis may be associated with joint symptoms (psoriatic arthritis). Medical assessment is important if joint pain or stiffness develops.
Care at Auria Dermatology Clinic is consultation-based and focused on accurate diagnosis and individual needs. Management plans are personalised, taking into account the type of psoriasis, symptom severity, and lifestyle considerations.